Introduction
Warts occur when the human papilloma virus enters the superficial layer of the skin in one spot, cells multiply and enlarge leading to a protruding lump. This we commonly term a “wart”.
The medical term “verrucae” means the same as “warts”, but few lay people likely would know that. I will stick to the more popular term “wart” in this summary. Depending on location there are a number of different types of warts.
Also, as the various cell types have different cell metabolisms, papilloma viruses adapted throughout the centuries and there are now more than 60 different papilloma virus types known that cause the various wart types. Here is an abbreviated list of some common warts and the types of papilloma viruses that cause them.
Various warts and their causes
| Name of wart: | Human papilloma virus type: | Comments: |
| Common warts | 1, 2, 4 and 7 | On hands, feet and around nail folds |
| Genital warts | 6, 11, 16, 18 and 33 | Strong association to cancer of the cervix in women and to bowenoid papulosis of genitalia in both sexes |
| CIN (=cervical intraepithelial neoplasia) of the cervix | 16, 18, 31, 33, 35 and 39 | These microscopic CIN III lesions are irreversible and lead to cancer of the cervix in women |
| Laryngeal papillomas | 6, 11, 16 and 30 | Can become cancerous; infants can acquire this from HPV in vaginal secretions during delivery; adults can get it from oral-genital sex |
| Flat warts | 3 and 10 | Common in children and younger adults, often in face |
| Heck’s disease (=oral papillomatosis) | 13 and 32 | Benign; treatment with CO2 laser |
Signs and symptoms
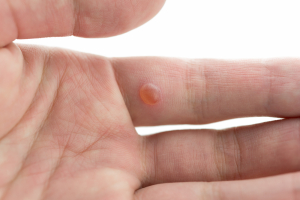
Wart lesions are sharply demarcated skin lesions with a cauliflower-like surface on top. Inside they are vascular and if injured can bleed a fair bit. They tend to grow slowly, but due to the fact that they do not hurt, might grow to a considerable size before they are detected. Here are several wart pictures.
If there is a point bleeding into the surface of the wart there might be a black component to the otherwise greyish appearance of the wart and the patient likely then will bring this to the attention of the physician for fear of cancer. In the nail-fold regions the warts may appear waxier, on the body skin surface they are drier.
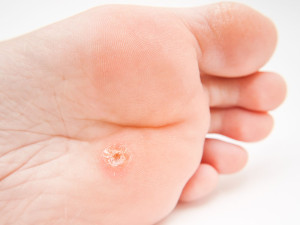
Plantar warts
On the sole of the foot, where the skin is thicker, the wart stays flat in appearance, but has a growth pattern that goes into the depth and only becomes apparent after several treatments with liquid nitrogen or several chemical applications followed with shaving using a surgical blade.
Diagnosis
The diagnosis in clinical practice is almost exclusively done by inspection and based on clinical experience. Here is a plantar wart picture. However, in certain high risk settings there are hybridization techniques available to separate oncogenic DNA from HPV’s, but this is only available in highly specialized research facilities. If this is not available, then a reasonable alternative is to treat warts conventionally first, and if they do not respond, to refer the problem lesions for further testing to a dermatologist.
Wart treatment
There are many effective treatment modalities, but all of them have a certain failure rate. Often it is not the failure of the treatment, but failure to treat the wart completely and to not repeat the treatments until the wart has been completely eradicated. Here are a few rules regarding wart treatment.
1. The most common therapy is to apply a salicylic acid daily onto the wart until it melts away slowly. Several preparations are available. Popular ones are such brand names as Duofilm and Duoforte 27 for common warts, and Duoplant for plantar warts.
2. If this fails, the physician may want to treat the warts with liquid nitrogen.
This method is used to freeze the wart, but not the surrounding skin for several seconds up to 15 or 30 seconds depending on the size and the type of wart. Under treatment will not have much effect on the wart, over treatment leads to painful blistering. The patient should be told to return after 1 or 2 weeks for a recheck. At the follow-up visit the physician may want to use a scalpel and peel the dead wart tissue down to the live wart. This is visible by the small punctuate bleeding spots from the wart vessels. At that level the wart is frozen again with liquid nitrogen and the procedure of recheck and possible repeat treatment with liquid nitrogen is done again. Using this method until eradication of all warts has a high success rate.
3. In case of resistant warts to the other treatment modalities it is useful to switch to a different treatment modality. Podofilox (brand name: Condyline), an antimitotic agent, causes the wart to shrivel up and fall off. It can also be combined with liquid nitrogen. Venereal warts on the outside of the male and female genitalia can be treated with Podofilox as well.
4. Laser surgery using a CO2 laser is useful in plantar warts and genital warts. However, scarring can result from this as it can with electric cautery.
5. Various anti-DNA chemicals such as topical 5-flourouracil (=5FU)has been used with success for flat warts as a 1% or 5% cream. Flat warts might also respond to tretinoin cream 0.05% (brand name: Retin-A 0.05% cream).
If a wart problem cannot be successfully treated by the family doctor, the patient should be referred to a dermatologist who has more experience in the difficult to treat wart cases.
References:
1.The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 265.
2.James Chin et al., Editors: Control of Communicable Diseases Manual, 17th edition, 2000, American Public Health Association
3.The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 112.
4. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 115.
5. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 113.