Introduction
Impetigo is a superficial skin infection, usually due to Staphylococcus aureus, a common pus producing bacterium.
However, in some cases group A beta-hemolytic streptococcus can be found. The lesion of impetigo is a blister like pustule. However, when this breaks open another form of impetigo can manifest itself, namely an ulcerative form, called “ecthyma” by dermatologists.
Signs and Symptoms
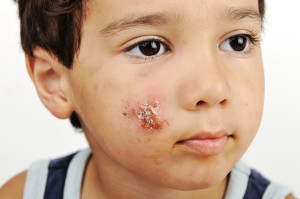
The lesions usually occur on arms and legs with children. The size of the lesions can vary from the size of a pea to a lesion of several centimeters in diameter with honey colored crusted edges. The lesions are itchy and this likely is the reason that it spreads as the bacteria are massaged into the healthy surrounding skin from scratching. Impetigo can be fairly localized as in this boy’s face or when not treated initially can be fairly widely distributed as shown in this link to a site with a picture of impetigo (thanks to hardinmd.lib.uiowa.edu for this image).
Diagnosis and Prognosis
Diagnosis is done clinically, but if doubts exist about the underlying pathogen, then a skin swab of the affected area can be made and sent for culture and sensitivity. The outcome, if treated quickly is very good with no problems of scarring. However, the longer the skin infection is left untreated, the more permanent skin scarring and pigmentation can result from impetigo. Also, with cases where group A beta-hemolytic streptococcus is found, there is a high incidence of a kidney disease called glomerulonephritis, if it is not treated right away with antibiotics. This is more common in children. It can leave the patient with permanent kidney damage.
Impetigo Treatment
Mupirocin (brandname: Bactroban) is applied topically 3 to 4 times per day to the affected skin. This is best complemented by oral administration of cloxacillin or cephalexin for 7 to 10 days to interrupt the cycle of reinfection (Ref. 1, p.2319 and Ref. 2, p.464).
References
1.The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 163.
2.James Chin et al., Editors: Control of Communicable Diseases Manual, 17th edition, 2000, American Public Health Association.
3.The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 164.
4. Feldman: Sleisenger & Fordtran’s Gastrointestinal and Liver Disease, 7th ed., © 2002 Elsevier : pages 1306-1307.