Introduction
Flesh eating disease conjures up an immediate image from newspaper articles and TV shows. Notably, in medical terms this condition has the name necrotizing fasciitis or necrotizing cellulitis. Its cause is the bug, Streptococcus pyogenes, which belongs into the group A Streptococcus type of bacteria and is also the cause of cellulitis. To point out, the difference is that with cellulitis the infection is on the surface of the skin. It is important to realize that with flesh eating disease the infection is in a deeper skin layer where the anatomy is softer.
Protein digesting enzymes are eating their way through the fascia
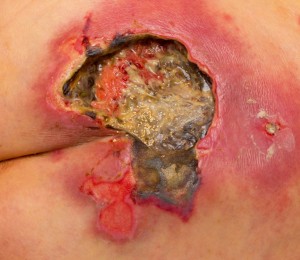
Once the bacteria have broken through the protective skin layer, they can spread very rapidly due to protein digesting enzymes eating their way through the fascia, which is located just below the subcutaneous tissue of the skin, and into the muscles and tendons. Once the fascia is liquefied with these enzymes, the bacteria have ideal growing conditions and multiply rapidly. It is extremely important to recognize that hours count in terms of early detection and swift initiation of surgical and intravenous antibiotic therapy. In the beginning there might be a deep skin ulceration as seen on the image here. But in the next hours or 1 to 2 days this type of skin ulceration when untreated could turn into the deep open wound in the lower leg region as shown in the link below.
Flesh Eating Disease
Signs and Symptoms
There is usually acute local pain in the area where the infection is. There is swelling in the overlying skin, it has a red color and is hot. With further deterioration there can be blistering and the color gets more of an angry looking appearance with a violet tinge to it. With touching there is sometimes a grating or crackling sensation that can be felt (medically termed “crepitation”).
There is a fever, fast heart beat and the patient’s level of consciousness may change from initial drowsiness to confusion and finally slip into a coma. Blood pressure drops due to loss of blood volume into the infected area.
Diagnosis and Prognosis
Even with the best intervention there is a mortality rate of 30%! It is important to do tests rapidly and to start therapy right away. X-rays often show gas formation from bacteria in the soft tissues. If it appears that there is pus under pressure, it is important to have a surgeon open this area for adequate drainage. Prior to that the physician might take a needle aspirate for Gram staining, or a swab taken during surgery can be sent off for that. Routine blood tests are taken for kidney and liver function tests as well as a coagulation screen to rule out other diseases and to gage the severity of this condition.
Treatment
Intravenous fluid replacement is given as large quantities of fluid have been lost into the infected region. The surgeon will do a generous exploration and wide opening of pus pockets to allow all of the infection to drain. In some centers where hyperbaric chamber treatments are available less debridements are necessary and better survival has been achieved.
At times an arm or a leg has to be partially or totally amputated just to save the person’s life. This is an area of medicine, which is cruel and gruesome! Nevertheless, in the last decade physicians made great progress in treating this life threatening condition. Apart from surgery, intravenous antibiotic treatment consisting of gentamycin, clindamycin (often in combination) or cefoxitine alone. Later the antibiotic is switched based on sensitivity results from the lab testing (Ref. 3, p.797 and Ref. 2, p.472).
References
1.The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 265.
2.James Chin et al., Editors: Control of Communicable Diseases Manual, 17th edition, 2000, American Public Health Association
3.The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 112.
4. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 115.
5. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 113.
6. Suzanne Somers: “Breakthrough” Eight Steps to Wellness– Life-altering Secrets from Today’s Cutting-edge Doctors”, Crown Publishers, 2008