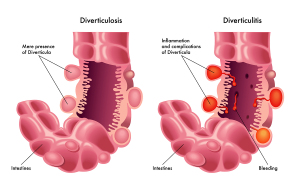
Introduction
First of all, the opening of a diverticle that experiences inflammation, can get so swollen that the diverticle forms a closed chamber. Then bacteria of the colonic flora multiply in there. In other words, the diverticle now has an infection, it is a diverticulitis. Finally, this can quickly turn into a diverticular abscess through the action of the E.coli bacteria. In addition, when the wall of the diverticle ruptures this causes acute peritonitis, or how surgeons call it”an acute abdomen”.
Fortunately, the patient has mostly a lot of symptoms of pain and a high fever when there is diverticulitis. In a word, the physician treats the patient in the hospital setting with the help of antibiotics to heal the diverticulitis. On the contrary, this avoids the abscess stage and prevents bowel perforation and peritonitis.
Symptoms and diagnosis
It must be remembered that most of the time the diverticular disease is ordinarily located in the sigmoid colon (left descending colon). In this case the patient presents with acute pain in the left lower abdomen. Associated with this is usually a fever. In addition, if the patient had a similar episode before, the physician likely would know that there is underlying diverticulosis and the diagnosis of diverticulitis can then be made fairly quickly. Equally important is that other causes of abdominal pain and fever have to be ruled out. For the most part, these are conditions like acute appendicitis, ovarian cancer or colon cancer to name a few. Occasionally a pericolic abscess can develop with severe chronic diverticular disease. All things considered, in time this can lead to bowel obstruction.
Treatment
Given these points, milder cases are obviously treated with antibiotics at home and repeat evaluation in the office setting. For the most part, more severely ill patients are usually admitted to the hospital and intravenous fluids and antibiotics are given. Whenever the patient is in hospital with an infection, blood tests are also done.
Generally speaking, about 2 weeks after the acute phase is over, a Barium enema with contrast can be done. Alternatively the physician can arrange a colonoscopy, if this is available. In either case a CT scan and/or ultrasound may still be necessary to check for a pelvic abscess in case of a persistent fever.
In a word, about 80% of patients can be treated conservatively. For the most part about 20% of patients need a surgical excision of the diseased segment of the colon or else a laparotomy to rule out more serious disease.
Special management of different cases with diverticulitis
First, a patient with an acute perforation and peritonitis will need the perforated piece of colon removed. In essence, this involves a preliminary proximal and distal colostomy. Second, at a later stage (2 to 6 months later) the surgeon does an end-to-end reconnection. Given these points, the danger after peritonitis is the extensive scarring. In the long run this can in future lead to recurrent bowel obstructions. Frequently the surgeon has to solve this with further surgery again. Mixed into all of this is the constant worry in the elderly patient that sooner or later colonic or other cancers may develop. In the meantime, the physician will always have to do supplementary tests to rule out this possibility.
References
1. M Frevel Aliment Pharmacol Ther 2000 Sep (9): 1151-1157.
2. M Candelli et al. Panminerva Med 2000 Mar 42(1): 55-59.
3. LA Thomas et al. Gastroenterology 2000 Sep 119(3): 806-815.
4. R Tritapepe et al. Panminerva Med 1999 Sep 41(3): 243-246.
5. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapters 20,23, 26.
6. EJ Simchuk et al. Am J Surg 2000 May 179(5):352-355.
7. G Uomo et al. Ann Ital Chir 2000 Jan/Feb 71(1): 17-21.
8. PG Lankisch et al. Int J Pancreatol 1999 Dec 26(3): 131-136.
9. HB Cook et al. J Gastroenterol Hepatol 2000 Sep 15(9): 1032-1036.
10. W Dickey et al. Am J Gastroenterol 2000 March 95(3): 712-714.
11. M Hummel et al. Diabetologia 2000 Aug 43(8): 1005-1011.
12. DG Bowen et al. Dig Dis Sci 2000 Sep 45(9):1810-1813.
13. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999.Chapter 31, page 311.
14. O Punyabati et al. Indian J Gastroenterol 2000 Jul/Sep 19(3):122-125.
15. S Blomhoff et al. Dig Dis Sci 2000 Jun 45(6): 1160-1165.
16. M Camilleri et al. J Am Geriatr Soc 2000 Sep 48(9):1142-1150.
More references
17. MJ Smith et al. J R Coll Physicians Lond 2000 Sep/Oct 34(5): 448-451.
18. YA Saito et al. Am J Gastroenterol 2000 Oct 95(10): 2816-2824.
19. M Camilleri Am J Med 1999 Nov 107(5A): 27S-32S.
20. CM Prather et al. Gastroenterology 2000 Mar 118(3): 463-468.
21. MJ Farthing : Baillieres Best Pract Res Clin Gastroenterol 1999 Oct 13(3): 461-471.
22. D Heresbach et al. Eur Cytokine Netw 1999 Mar 10(1): 7-15.
23. BE Sands et al. Gastroenterology 1999 Jul 117(1):58-64.
24. B Greenwood-Van Meerveld et al.Lab invest 2000 Aug 80(8):1269-1280.
25. GR Hill et al. Blood 2000 May 1;95(9): 2754-2759.
26. RB Stein et al. Drug Saf 2000 Nov 23(5):429-448.
27. JM Wagner et al. JAMA 1996 Nov 20;276 (19): 1589-1594.
28. James Chin, M.D. Control of Communicable Diseases Manual. 17th ed., American Public Health Association, 2000.
29. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 157, page1181.
30. Textbook of Primary Care Medicine, 3rd ed., Copyright © 2001 Mosby, Inc., pages 976-983: “Chapter 107 – Acute Abdomen and Common Surgical Abdominal Problems”.
31. Marx: Rosen’s Emergency Medicine: Concepts and Clinical Practice, 5th ed., Copyright © 2002 Mosby, Inc. , p. 185:”Abdominal pain”.
32. Feldman: Sleisenger & Fordtran’s Gastrointestinal and Liver Disease, 7th ed., Copyright © 2002 Elsevier, p. 71: “Chapter 4 – Abdominal Pain, Including the Acute Abdomen”.
33. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.