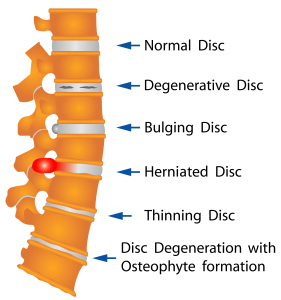
Generally speaking, degenerative disc treatment suggestions have to be understood with the knowledge that there are significant changes in the spine as we age. Specifically, there is a drying up of the disc material and of the lubrication of the joint fluid in the facet joints. To clarify, the facet joints are the row of small joints on each side of the spinal canal, which together with the discs as a unit give the spine its mobility.
In particular, with degenerative changes there are bone spurs, there is loss of joint space and a general stiffening and a painful decrease of range of motion. Ultimately these changes can eventually be seen on X-rays and the drying out of the discs, called “desiccation” can be visualized on an MRI scan. Obviously, to prevent this from happening prematurely fitness walking, stretching exercises and mild to moderate weight training programs are useful.
Premature degenerative changes
However, heavy weight training, conversely, can accelerate the wearing out of the facet joints and discs thus leading to premature degenerative changes. Similarly, multiple sports injuries, car accidents or fights will also accelerate this type of degenerative arthritis, typically with a 5 to 10 year delay following a back injury.
Furthermore, anti-inflammatory medication such as the COX-2 inhibitors or regular non-steroidal anti-inflammatories will help to control the inflammation and allow the patient to do the gentle reconditioning that is required. In conclusion, heat treatment, acupuncture and massage treatments and swimming are all useful therapeutic modalities.
End stage degenerative arthritis
However, for the most part in more severe cases where the degeneration of the facet joints has progressed to the point that bone rubs on bone, surgery may be indicated. Similarly, when the disc material has been thinned out to the point where one vertebral body almost rubs on the other, this, too, would require back surgery. Typically, the surgeon takes a bone graft from the pelvic bone and fuses the degenerative joint or the disc space. That is to say, in medical circles it is called “spinal fusion surgery”. Indeed, the orthopedic or neurosurgeon will be able to advise whether or not this is an option in a particular patient. Every patient has to be judged according to the individual circumstances.
References
1. ABC of rheumatology, second edition, edited by Michael L. Snaith , M.D., BMJ Books, 1999.
2. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 52.
3. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 275,p.2429.
4. HA King Orthop Clin North Am 1988 Apr;19(2):247-255.
5. HA King Orthop Clin North Am 1999 Jul;30(3):467-474, ix.
6. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 59.
7. JA Smith Orthop Clin North Am Jul 1999; 30(3): 487-499.
8. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 56, p. 469.
9. Wheeless’ Textbook of Orthopaedics: http://www.wheelessonline.com/
10. Goldman: Cecil Textbook of Medicine, 21st ed.(©2000)W.B.Saunders
11. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
12. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevier