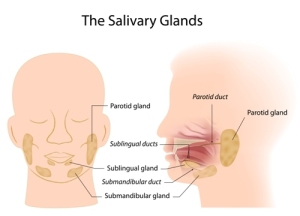
In the older patient salivary gland stones occur with a higher frequency.
In patients who have a tendency for gout, the frequency of parotid gland stones is even higher. Essentially these stones come from calcium or uric acid salts that precipitate in the ducts of the parotid and submandibular glands. Parotid gland stones occur in about 20%, submandibular gland stones in 80% of all salivary gland stones.
Symptoms
There are enlarged salivary glands, particularly with eating as more digestive juices are produced, but get congested behind the stone that plugs the parotid gland or submandibular gland duct. The pain can get so severe that the term “salivary colic” was coined to describe it medically (Ref. 8). Because there is congestion and a lot of digestive enzymes in the ducts, bacteria find their way into the duct and tissue, and painful local abscesses and local bacterial parotitis develop. Even when this is successfully treated with antibiotics, a vicious cycle of scarring, congestion, and further development of stones in the salivary duct with more infections may develop.
Diagnostic Tests
According to Ref. 8, p. 822, intraoral radiographs and occlusal X-ray views detect up to 94% of all stones. CT scanning and sialograms (where the ducts are filled with a contrast material followed by X-rays, thanks to adam.com for image) complete the work-up. With those patients who are allergic to contrast material ultrasound examination can detect up to 90% of the stones that are larger than 2mm in diameter (Ref.8).
Treatment
The newest parotid gland stone treatment is shock wave lithotripsy (extracorporal lithotripsy = ECL). This technique has been successfully employed to break kidney stones down to the size of sand like particles, which can be passed naturally. With parotid gland stones the same technique has been successfully adapted and this should likely be attempted first before the conventional surgical approach would be employed. According to Ref. 8 more than 50% of parotid gland stones can be treated successfully with ECL. Submandibular gland stones have to be treated with conventional surgery as ECL is not that successful.
References:
1. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 84.
2. Noble: Textbook of Primary Care Medicine, 3rd ed.,2001, Mosby Inc.
3. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 85.
4. Rakel: Conn’s Current Therapy 2001, 53rd ed.,2001, W. B. Saunders Company
5. Goldman: Cecil Textbook of Medicine, 21st ed.,2000, W. B. Saunders Company
6. Mandell: Principles and Practice of Infectious Diseases, 5th ed.,2000, Churchill Livingstone, Inc.
7. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 265.
8. MF Williams: Otolaryngol Clin North Am; Oct1999; 32(5): 819-834.
9. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 106.
10. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
11. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevier