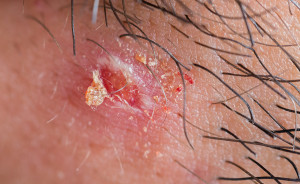
Introduction
Acne vulgaris affects the oil glands of the skin. It must be remembered that the secretions appear to be more tenacious than in normal controls. Notably, on the one hand it is a hereditary disease, but on the other hand hormonal imbalance plays a triggering role for worsening of acne. In this case, adolescence is usually the time when the teenager is affected with acne. That is to say, the peak is when they enter puberty and many are improved a few years later except for those who have a genetic trait, in which case it can take 5 or 10 years before substantial relief is noticed.
Interplay between oil glands, androgens and acne bacteria
Chiefly, the underlying disease process is a complex interaction between oil glands, androgens in males (but also in acne prone females) and acne bacteria leading to free fatty acids from lipases released from the bacteria. Indeed, all of this leads to an inflammatory reaction of the oil gland and duct. The result is the formation of comedones, black heads, which plug the oil ducts and lead to further multiplication of other pus forming bacteria and this ends up in mini abscesses, called pustules (whiteheads).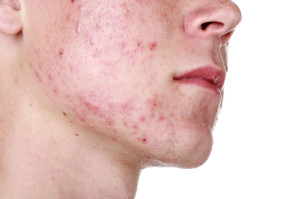
With this in mind, these can lead to a deeper skin abscess and even to carbuncles. Unfortunately these leave scars behind (dimples in the skin), which will be noticeable for years to come, even if the initial acne process with inflammatory lesions normalizes later in life.
Acne in women
In women acne is often associated with an accumulation of male hormone precursors in the blood, which changes the body hair distribution called hirsutism, with male type hair distribution and scalp hair loss (=alopecia). In general, in women who develop acne there often is a family history of severe acne in at least one of the parents’ sides.
Signs and symptoms
To point out, the basic acne lesion is the comedone, which is a skin pore plug composed of old thickened skin oil. If it is non-inflamed, it does not do damage, but looks unsightly (light brown first, weeks later dark and even black). The following table explains some of the terminology that acne patients will hear from physicians:
Acne vulgaris terminology
| Medical terms: | Comments: |
| comedone | “blackhead”, a thickened oil plug |
| pustule | “yellow head”, a mini abscess just below the comedone |
| papule | ‹5 mm (=1/5″) in size, a local inflammatory reaction giving the skin a raised appearance |
| nodule (or cyst) | ›5mm (=1/5″) in size, itching, burning cystic lesion, which the patient wants to squeeze |
| sinus tract | repeat healing over and rebreaking of chronic cysts leads to sinus tract formation underneath the skin and scarring |
Diagnostic tests
Depending on whether the acne is mild, moderate or severe, there are several Latin names that dermatologists have developed over the decades to describe exactly what type of acne the patient has. Some of these names are: nodular acne, acne fulminata, acne conglobata etc. In modern times these names have become somewhat meaningless as it turns out that the underlying disease process is the same for the mild or severe cases of acne. The more severe cases are the ones where genetic factors and male hormone factors are more prominent.
Arrival of isotretinoin
However, since the advent of isotretinoin (brandname: Accutane Roche) the more severe cases are treated with this medicine, whereas the other milder cases can be treated with the conventional methods from the past.
As in many other skin diseases this skin condition is entirely diagnosed by history and clinical appearance. This depends on the experience of the physician. Most cases can easily be handled by the family doctor, but the more chronic and severe cases should be referred to a skin specialist (dermatologist) for assessment and treatment.
Treatment
There are a number of treatment modalities. Peeling agents such as benzoyl peroxide (brand names: PanOxyl, Solugel, Acetoxyl, Benzagel Acne Gel etc.) are put on as gels or creams once at bedtime or twice per day. If the concentration is too strong for the skin (every skin type has a breaking point), it gets irritated and looks like a sunburn. These agents soften the comedones, unplug the oil gland ducts and allow for a normal oil gland flow while at the same time disinfecting the skin surface as they are suppressing the growth of P. acnes, the bacterial culprit of acne.
Antibiotics can help acne
The skin specialist often combines peeling agents with oral antibiotics such as erythromycin or tetracycline for a period of time. Tetracycline and similar medications cannot be taken in pregnancy as they cause congenital anomalies. In milder cases topical antibiotic therapy with clindamycin, sulfonamides or erythromycin applied at bedtime is another option. Other useful topical therapy is tretinoin (brandname: Retin A), which comes in different concentrations. This is Vit. A acid and works by liquefying the skin surface and dissolving comedones thus preventing the further development of pustules, papules and nodules. Side-effects are reddening of the skin, burning and drying of the skin. The key is to find out the right concentration that the patient tolerates.
Isotretinoin liquifies oil gland secretions
Finally for the moderate and severe acne patient the gold standard therapy has become isotretinoin (brand name: Accutane Roche). These are capsules that are taken by mouth. The medication works from inside by liquefying the secretions of the oil glands and opening up the oil gland ducts. Usually, the physician puts the patient with acne on a course of 12 to 16 weeks of treatment. The effect of suppressing acne can last for several months and up to one year. When it comes back, a boost treatment of 3 to 6 weeks can often stabilize it for an equally long period of time.
Side effects of isotretinoin
Ask your physician about side-effects. Pregnant women cannot take this medication as it would cause severe genetic abnormalities in the fetus in more than 25% even in short term doses. There are significant side-effects in terms of dry itchy skin, dry nose, facial dermatitis and others. Newer medications are under investigation that address the inflammatory reactions in the hair follicles.
UV light therapy for acne
Another adjunct to acne treatment can be acne blue light therapy (=UV light). It is an old observation that acne patients get better with their acne in summer when they get sun exposure. However, the side effect of the treatment potentially is possible higher risk for skin cancer in decades later.
Do not neglect the healing effect of a sensible diet. Skin specialists identified milk allergies, overuse of saturated fats and sugar as the culprits for causing acne.
For more information on the effect of diet regarding acne see these blogs:
http://www.askdrray.com/dietary-habits-help-for-clear-skin/
http://www.askdrray.com/pimples-and-acne-can-be-caused-by-food/
http://www.askdrray.com/diet-can-influence-acne/
References
1. Habif: Clinical Dermatology, 3rd ed.,1996, Mosby-Year Book, Inc.
2. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 117.
3. Cotran: Robbins Pathologic Basis of Disease, 6th ed.,1999, W. B. Saunders Company
4. Noble: Textbook of Primary Care Medicine, 3rd ed., 2001, Mosby, Inc.
5. Rakel: Conn’s Current Therapy 2001, 53rd ed., 2001, W. B. Saunders Company
6. Goroll: Primary Care Medicine, 4th ed., 2000, Lippincott Williams & Wilkins
7. Richard J. Lewis, M.D. at the 42nd Annual St. Paul’s Hosp. CME Conf., Nov.1996, Vancouver/BC
8. Jerry Shapiro, Prof. Dermatol., UBC, at 45th Annual St. Paul’s Hosp. CME Conf., Nov.1999, Vancouver/BC
9. D Seager Int J Cosmet Surg Vol 6, No. 1, 1998: 27-31.
10. Townsend: Sabiston Textbook of Surgery, 16th ed.,2000, W. B. Saunders Company
11. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
12. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevier