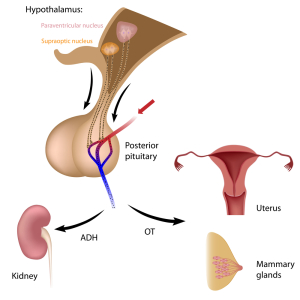
Central Diabetes Insipidus (central DI) can be inborn from a hypothalamic hamartoma (thanks to radiopaedia.org for this link) where hypothalamic hormone production and subsequently ADH (antidiuretic hormone) production is diminished.
Not infrequently it can also be acquired as Ref. 5 reviewed. This reference shows that MRI studies can be useful to follow these patients. The causes for this can be quite varied and include metastasizing tumors, trauma (basal skull fracture), brain sarcoidosis, brain tuberculosis, cerebral aneurysms and destructive hypothalamic lesions from meningitis or encephalitis.
Finally there is a rare genetic abnormality of the vasopressin gene on chromosome 20, which is responsible for an autosomal dominant form of a familial diabetes insipidus. However, apart from the cases mentioned above, most cases still remain unexplained as to why they occur.
Symptoms
The two cardinal symptoms as mentioned in the introduction chapter on DI are polydipsia (excessive thirst and fluid intake) and polyuria (frequent trips to the bathroom with immense amounts of urine). The urine is very diluted and if osmolality is measured, it is less than 200 mOsm per liter. The patient has to go to the bathroom at nights as well (nocturia) contrary to psychogenic water drinking.
Diagnosis
The simplest way to diagnose central DI is in the hospital setting by way of the water deprivation test. This test consists of a period of fluid deprivation, which in normal persons would lead to urine concentration.
However, in central DI patients the urine osmolality never exceeds that of the plasma osmolality.
When vasopressin is give by injection, the normal person would only increase the urine osmolality by an additional 5%, whereas the central DI would concentrate it now by more than 50%. In contrast, a patient with nephrogenic DI would not show any response of the urine osmolality to the vasopressin injection.
Treatment
Hormone replacement therapy with a vasopressin analogue is the treatment of choice. In the past vasopressin had to be given several times per day by needle subcutaneously.
This was necessary as the regular vasopressin wears off in 6 hours or less. However, all of this changed with the arrival of desmopressin acetate, or DDAVP.
This is an acronym for a complicated chemical name of an arginine derivative of vasopressin that lasts for between 12 and 24 hours and can be given by nasal spray (Desmopressin nasal spray, brand names: DDAVP, Stimate, Minirin). Each puff delivers 10 micrograms of DDAVP and most people need only one puff in the morning and one puff in the evening. It is well tolerated and normalizes the life of a patient with central DI. It is also available by injection. Side effects can be high blood pressure and hyponatremia (when overdosed, see Ref. 10).
Prognosis
As long as the central DI is not due to an incurable tumor, life expectancy with the use of the DDAVP nasal spray for such a patient is normal.
References:
1. MT Kailasam et al. J Hypertens 2000 Nov 18(11): 1611-1620.
2. G Chinetti et al. Inflamm Res 2000 Oct 49(10): 497-505.
3. St. Paul’s 46th Annual Cont. Med. Educ. Course for Prim. Phys., Nov. 14-17, 2000. Dr. David Thompson, Div. of Endocr., Vancouver Hosp. and UBC.
4. B J Goldstein Int J Int Pract 2000 Jun 54(5): 333- 337.
5. M Maghnie et al. N Engl J Med 2000 Oct 5;343(14): 998-1007.
6. E Albertazzi et al. J Am Soc Nephrol 2000 Jun 11(6):1033-1043.
7. M Funk et al. American Journal of Emergency Medicine Vol.19,No.6, Oct.2001, W. B. Saunders Company
8. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
9. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevie
10. http://en.wikipedia.org/wiki/Desmopressin