Introduction
Let me start this glaucoma overview by stating that glaucoma is the second most common reason for loss of eyesight in the US. The first reason for loss of eyesight in the US is macular degeneration. There are about 2 million Americans who have glaucoma, but only about 50% know about it. It can hit at any age group, although it is more common in the older age group.
Among younger glaucoma patients some inheritance of glaucoma occurs more often. Alternatively, there was prior injury to the affected eye leading to internal scarring. Of those who have high intraocular pressure (=IOP) only 1% per year will develop glaucoma. There are two forms, the open-angle glaucoma found in about 70% and the angle-closure glaucoma, which occurs in about 10% of all cases.
Four crucial eye examination tests
The remaining 20% are more difficult to classify. Usually, glaucoma develops from a blockage of the Schlemm’s canal. This is shown in this image where on the left conditions are seen with normal eye pressure and on the right when glaucoma is present. The eye fluid has no normal way of drainage when this happens and this will raise the IOP in most cases. In about 85% of cases the IOP will be elevated. But in about 15% of glaucoma patients the IOP is normal when the IOP is measured. An ophthalmologist will, however, do 4 tests that will determine whether or not the patient has glaucoma:
- Eye exam including gonioscopy
- Measuring intraocular pressure
- visual field examination
- examination of optic discs (using slit lamp)
Only when the eye specialist examines all these four parameters, can the eye specialist tell whether there is glaucoma present that needs treatment.
Avoiding glaucoma misdiagnosis
Otherwise glaucoma could be missed or get overdiagnosed. Here are two examples: a normal or low-pressure glaucoma patient could be overlooked, if only the IOP is measured. This patient would wrongly miss treatment for glaucoma, which would lead to blindness on that eye from optic nerve atrophy. Another example is a patient with an elevation of the IOP (intraocular pressure, ocular hypertension). This patient would receive a false diagnosis of glaucoma, if the eye specialist only measures the IOP.
In this case the other 3 examination methods would rule out glaucoma and the correct diagnosis would be “ocular hypertension”. 90% of patients with ocular hypertension (IOP more than 21 mm mercury) will not develop glaucoma and simply need regular follow-up exams for monitoring. On the other hand, if these patients develop IOP’s of greater than 28 mm mercury, many eye specialists would start treating these patients with eye drops to lower the IOP, as these patients likely were in the early stages of glaucoma development.
There are high risk groups who develop open-angle glaucoma as I describe below.
Common causes of open-angle glaucoma
| Family history | diabetes |
| older age | high blood pressure |
| elevated IOP | conditions that requires chronic use of systemic corticosteroids |
| black race | Myopia (shortsightedness) |
Signs and symptoms of glaucoma:
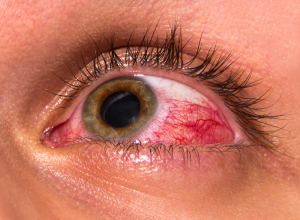
Unfortunately there are no early signs and symptoms for glaucoma. Late symptoms are loss of the visual fields in the sense of missing words or lines when reading or missing stairs when the lower visual field is missing. This can cause accidents when driving a car. First the vision in the periphery disappears, later central vision vanishes. Other symptoms can be blurred vision and intermittent eye pain.
In this glaucoma overview I will briefly touch on the following topics.
Diagnostic tests
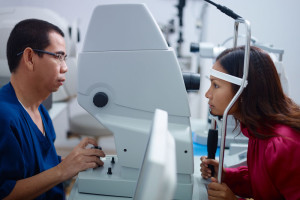
As already indicated the eye specialist will do a thorough eye examination including gonioscopy and measurements of the intraocular pressure (IOP) where one of the methods is the Goldmann tonometry. In addition, as mentioned above, the specialist will also do visual field exam and do slit lamp examination to inspect the optic disc.
Treatment of glaucoma
Both surgical glaucoma procedures will restore the normal drainage of the internal eye fluid, which in turn takes the pressure off the optic nerve. In most open-angle glaucoma patients laser surgery can be done by an eye surgeon equipped to do that procedure. The eye specialist does conventional surgery only in those cases where the specialist cannot use laser surgery. Here is another site where glaucoma surgery is described.
Prevention of glaucoma
To prevent glaucoma, it is important that an eye specialist examines the patient from age 30 onwards every 2 or 3 years. The optometrist or ophthalmologist does examinations more often in high risk families where there is glaucoma inheritance. This way the health professional detects early changes and can treat right away with laser surgery. High risk people (see in the table above) require careful checking and close follow-up.
References
2. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
3. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevier