Introduction
Treatment of a heart attack is important to minimize complications after a heart attack.
It is important to treat this condition right away from the beginning due to arrhythmias, heart failure and hypotension, which could turn into cardiogenic shock and death due to further a further compromise of blood flow to the heart muscle.
Treatment therefore would include arrhythmia medications (Xylocaine and others), water pills (=diuretics), oxygen therapy and possibly thrombolytic therapy such as streptokinase and others. A Swan-Ganz catheter might have to be placed in the right heart to measure pressures inside the heart and to be able to know exactly how much of each of the various specific heart medications to give. Obviously a cardiologist should supervise this kind of invasive, but often very successful therapy.
Only a few decades ago the overall mortality of people with heart attacks was about 60%. Now with good CPR initially and the Emergency Response Team being able to institute some of the therapy right at the scene and on the way to the hospital and with improved methods at the hospital the mortality rate has declined to 10 to 20 %. Obviously, the more the person neglected his/her health, the more serious the disease and the worse the mortality rate.
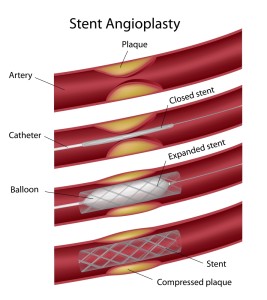
Several treatment methods are at the disposal of the cardiologist. First, reperfusion therapy can be achieved by fibrinolytic therapy or by percutaneous coronary intervention (PCI), also known as angioplasty. Fibrinolytic therapy is aimed at dissolving the clot in the affected coronary artery. There are a confusing array of fibrinolytic agents available, such as streptokinase, tissue-type plasminogen activator (t-PA), heparin and various newer agents. A 12 lead ECG tracing is done and patients are selected for fibrinolytic therapy on the following criteria: there has to be at least a 1 mm elevation of an ST segment (STEMI patients, see introduction) or there has to be a recent left bundle branch block (LBBB) on the ECG. Multiple trials have established that other patients who do not fulfill these criteria will not respond to fibrinolytic therapy (Ref. 10).
An early percutaneous (through the skin) transluminal (through the clot, but inside the lumen of the artery) cardiac angioplasty (=PTCA for short or PCI) can be as effective as blood clot dissolving (fibrinolytic) therapy. But the cardiologist will carefully select patients according to various criteria that have been developed through various clinical trials, so the optimal chance of survival is achieved.
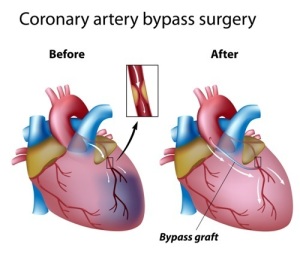
PTCA has saved many lives as has CABG, an acronym for “coronary artery bypass graft”. The cardiologist in consultation with a cardiovascular surgeon can judge what procedure is best suited for a particular patient.
PCI has to be done very early, preferably within 3 to 6 hours of onset of chest pain to be successful in rescuing heart tissue. If it is delayed, there is an alternative to “save some time” by putting patients on platelet inhibitors. The oldest one is aspirin (ASA). But there are more potent platelet inhibitors, namely the thienopyridines, ticlopidine and clopidogrel. One of these will likely be started. The purpose is to keep clotting under control. However, the downside is the complication of a hemorrhagic stroke. Age is no longer a criterion for exclusion of fibrinolytic therapy, but patients above the age of 75 do have a higher incidence of hemorrhagic stroke with a high death rate than younger patients do. Fibrinolytic therapy has to be initiated within 6 hours from the start of heart attack symptoms, at the latest within 12 hours, to be successful in reopening a clotted coronary artery. With the use of anti-platelet therapy (ASA, clopidogrel etc.) early on in the Emergency department the mortality rate has decreased by 25 to 50% (Ref.10).
What are some of the late complications following a heart attack?
Within the first year following a heart attack about 10 % will develop a further heart attack as more stenotic lesions in the coronary arteries develop. Others will develop sudden irregular heart beats which sometimes can be life threatening and difficult to treat. Another complication is congestive heart failure which needs to be treated with angiotensin converting enzyme( ACE) inhibitors. All of these complications require an assessment by a cardiologist (Ref. 9, p. 1668).
There is evidence that heart attacks can be prevented with 4000 mg of omega-3 fatty acids per day.
References
1. DM Thompson: The 46th Annual St. Paul’s Hospital CME Conference for Primary Physicians, Nov. 14-17, 2000, Vancouver/B.C./Canada
2. C Ritenbaugh Curr Oncol Rep 2000 May 2(3): 225-233.
3. PA Totten et al. J Infect Dis 2001 Jan 183(2): 269-276.
4. M Ohkawa et al. Br J Urol 1993 Dec 72(6):918-921.
5. Textbook of Primary Care Medicine, 3rd ed., Copyright © 2001 Mosby, Inc., pages 976-983: “Chapter 107 – Acute Abdomen and Common Surgical Abdominal Problems”.
6. Marx: Rosen’s Emergency Medicine: Concepts and Clinical Practice, 5th ed., Copyright © 2002 Mosby, Inc. , p. 185:”Abdominal pain”.
7. Feldman: Sleisenger & Fordtran’s Gastrointestinal and Liver Disease, 7th ed., Copyright © 2002 Elsevier, p. 71: “Chapter 4 – Abdominal Pain, Including the Acute Abdomen”.
8. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
9. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapters 197, 202, 205 and 207.
10. Marx: Rosen’s Emergency Medicine, Chapter 76 – Acute Coronary Syndrome; spectrum of disease. 7th ed. copyright 2009 Mosby, An Imprint of Elsevier
11. http://www.ncbi.nlm.nih.gov/pubmed/19891279 : Cziraky MJ, Watson KE, Talbert RL: “Targeting low HDL-cholesterol to decrease residual cardiovascular risk in the managed care setting.” J Manag Care Pharm. 2008 Oct;14(8 Suppl):S3-28; quiz S30-1.
12. http://www.ncbi.nlm.nih.gov/pubmed/23029021 : Hoevenaar-Blom MP, Nooyens AC, Kromhout D, Spijkerman AM, Beulens JW, van der Schouw YT, Bueno-de-Mesquita B, Verschuren WM: “Mediterranean Style Diet and 12-Year Incidence of Cardiovascular Diseases: The EPIC-NL Cohort Study.” PLoS One. 2012;7(9)
13. http://www.ncbi.nlm.nih.gov/pubmed/20236088 :Shecterle LM, Terry KR, St Cyr JA.: “The patented uses of D-ribose in cardiovascular diseases.” Recent Pat Cardiovasc Drug Discov. 2010 Jun;5(2):138-42.
14. http://www.ncbi.nlm.nih.gov/pubmed/19200398 : Sawada SG, Lewis S, Kovacs R, Khouri S, Gradus-Pizlo I, St Cyr JA, Feigenbaum H. “Evaluation of the anti-ischemic effects of D-ribose during dobutamine stress echocardiography: a pilot study.” Cardiovasc Ultrasound. 2009 Feb 7;7:5.
15. http://www.ncbi.nlm.nih.gov/pubmed/22040938 : Ferreira JC, Mochly-Rosen D. “Nitroglycerin use in myocardial infarction patients.” Circ J. 2012;76(1):15-21.
16. http://www.ncbi.nlm.nih.gov/pubmed/21530799 : Zand J, Lanza F, Garg HK, Bryan NS. “All-natural nitrite and nitrate containing dietary supplement promotes nitric oxide production and reduces triglycerides in humans.” Nutr Res. 2011 Apr;31(4):262-9.
17. http://www.ncbi.nlm.nih.gov/pubmed/22821988 : Christou DD, Pierce GL, Walker AE, Hwang MH, Yoo JK, Luttrell M, Meade TH, English M, Seals DR. “Vascular smooth muscle responsiveness to nitric oxide is reduced in healthy adults with increased adiposity.” Am J Physiol Heart Circ Physiol. 2012 Sep;303(6):H743-50.