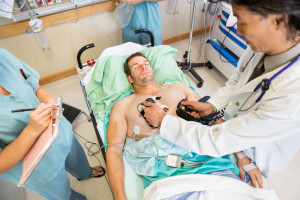
The initial phase of an myocardial infarction (=MI) is particularly vulnerable for developing arrhythmias post myocardial infarction until the scarred area in the heart muscle consolidates.
This usually takes until 7 to 10 days from the beginning of a heart attack. In the first 3 days following an MI this danger is highest and usually patients are kept in an Intensive Care Unit setting or a Coronary Care Unit of a larger hospital. There the patient is hooked up to the latest testing and heart monitoring.
Telemetry is a newer technology where the patient can mobilize, but is connected through radio waves to a central monitoring station. An intravenous hookup is in place so that in an emergency there is instant access to a vein and medication can be given very quickly. When dangerous irregular heart rhythms develop and are detected on the monitor screen, appropriate antiarrhythmic medication can be given intravenously, which then rapidly stabilizes an otherwise very precarious cardiac situation. The cardiac care nurse will check vital signs frequently in order to monitor the pump function of the heart.
Ventricular fibrillation
The worst scenario is the sudden occurrence of ventricular fibrillation. This is a deadly arrhythmia where the heart muscle fibers contract in a completely dissociated pattern so that the heart as a whole can no longer pump blood.
The patient becomes dizzy, then unconscious and would die in only a few minutes, if left alone. The health care providers in the Coronary Care Unit are prepared for this emergency and will quickly use a defibrillator where a pulse of electric current is administered via electric paddles, which are pressed against the skin of the chest wall. This depolarizes all of the heart muscle fibers and the electrical impulses originating in the sinus node can then start again, which makes the heart beat regularly on its own again. What a thrill it is for the health care workers when such a maneuver is successful! With no other underlying cause such a defibrillation procedure works miracles. It really can safe lives.
However, it has to be applied before the patient accumulates a lot of lactic and carbonic acid from a lack of breathing and before the heart muscle becomes too deplete of oxygen. In that condition the heart muscle does not want to respond and options are running out very quickly. Ambulance drivers today are trained to use portable defibrillators for emergencies such as these and this has improved the survival among heart attack victims significantly. Unfortunately many heart attack patients still die before they ever reach the hospital. It is only in the last decade that the idea of the emergency response team that carries some of the hospital equipment has caught on.
The U.S. and Canada have been pioneers in the introduction of this technology in emergency response teams outside of hospitals. Thousands of lives have already been saved that way and thousands more will be saved in future by bringing this service more and more to the rural areas. Call 911 when you see a person with a heart attack, a seizure or a stroke. Then the ambulance team can come and help to stabilize that person and rush him or her to the hospital where more medical help is available. In order to establish a “life chain” it is important that a significant percentage of the population knows cardiopulmonary resuscitation (CPR). This way a person in distress can be kept alive even when the heart is not beating on its own. Next the community emergency response team can diagnose what rhythm the patient’s heart is in using the modern equipment. This information will then dictate what therapy is instituted. In a straight forward case the ambulance attendant can proceed with the defibrillator. If things are more complex, information may have to be relayed to the hospital and a cardiologist may have to give radio instructions to the attendant on how to proceed further.
Often, by the time the ambulance arrives at the hospital, the patient is already stabilizing because the anoxia (lack of oxygen in the tissues) has been reversed. The underlying condition, which lead to the emergency, can then be addressed in the hospital setting. With such a life chain as just described the outcome has become much better. But without a preventative approach within the population the figures of success will not exceed the 50 to 60 % success rate on the long term. We have come a long way from figures of 5 to 10 % success in the past before the emergency response team was established. However, when people are overweight, smoke and do not exercise , the resulting disease process in the heart, lungs and blood vessels is so severe that the overall outcome even with the best emergency response team cannot be successful. Bad disease leads to bad results. Without good ingredients a cook cannot bake a good cake. Medicine is not any different: You need good basic tissues to have a good long term outcome (Ref. 1, p. 1710).
References:
1. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapters 197, 202, 205 and 207.
2. Braunwald: Heart Disease: A Textbook of Cardiovascular Medicine, 6th ed., 2001, W. B. Saunders Co.
3. D C Bauer: Audio-Digest Family Practice Vol. 49, Iss. 09, March 2, 2001.
4. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
5. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevier