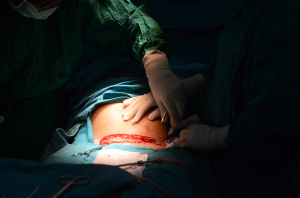
Abnormal labor and birth complications are anything that is different from what was described as normal earlier.
Often there can be a very fast transition from an apparently normal course to a completely abnormal one. For instance, the fetal heart beat could suddely slow to below 100 beats per minute with a contraction very early in the course of the delivery. If this persits, an emergency cesarean section might have to be done right away to rescue the baby.
On the other hand with different positioning the heart rate may recover, but the physician may want to insert an internal fetal heart monitor to monitor the heart rate more closely in relation to labor pains. At this time the is higher than initially when things were entirely normal.
The physician is now likely worried that there might be umbilical cord problems (possibilities: cord prolapse, umbilical cord compression with labor pains, umbilical cord knot that might tighten with further descent or too short a cord etc.).
“Why am I rushed to the operating room for an emergency cesarean section?”
In child delivery things are not always predictable. The heart beat can suddenly go down to dangerously low beats. The mother’s blood pressure can go suddenly up and she may seizure (eclampsia). In order to rescue the baby or the mother or both the physician may at times have to very quickly act and arrange for an emergency cesarean section, which by itself has a certain risk of mortality. Inaction in situations like this can have disastrous consequences for the baby or the mother. At times details of the circumstances may only be understood later when the physician can explain what had led to the emergency cesarean section.
If labor is well established and stage II is in progress with the woman pushing the baby out of the birth channel, a situation such as a reduction of the fetal heart rate may not be as ominous. As long as the fetal heart rate recovers between labor pains, the baby may not be in distress. In these situations the health care provider must decide in split seconds what is the “right thing to do” in this particular situation. It may be that nothing has to be done, perhaps some oxygen for the mother. But in another case it might be important to gain a few seconds or minutes for the sake of the baby’s brain development (lack of oxygen at this vulnerable stage is a major cause of learning disability) to rush the delivery along with a gentle forceps delivery. Contrary to what many people believe, a gentle forceps pull or a vacuum extraction with a bell applied to the baby’s head and assisted pulls during labor pains will not harm the baby’s head or neck (Ref. 18, p. 387).
Induction of labor
There are certain situations where it would be too risky to wait for spontaneous labor.
For instance in a high risk setting the specialist may decide to do a “fetal stress test” or “non stress test”, where 30 minutes of fetal monitoring are done with or without syntocinon. If the woman is close to her expected delivery date and the stress test looks like labor would be imminent, labor may then be induced with the help of a syntocinon drip. Ask your doctor for more details. This is only an emergency tool for the specialist, not a convenient way to end a normal pregnancy. Unfortunately, in the past it was fashionable among some obstetricians to have the delivery induced before the specialist went on holidays and many babies have been lost when the attempt failed. Failed inductions are a source of prematurely born babies and the overall risk of induced deliveries is higher than that of normal deliveries.
References:
1. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 235.
2. B. Sears: “Zone perfect meals in minutes”. Regan Books, Harper Collins, 1997.
3. Ryan: Kistner’s Gynecology & Women’s Health, 7th ed.,1999 Mosby, Inc.
4. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 245.
5. AB Diekman et al. Am J Reprod Immunol 2000 Mar; 43(3): 134-143.
6. V Damianova et al. Akush Ginekol (Sofia) 1999; 38(2): 31-33.
7. Townsend: Sabiston Textbook of Surgery,16th ed.,2001, W. B. Saunders Company
8. Cotran: Robbins Pathologic Basis of Disease, 6th ed., 1999 W. B. Saunders Company
9. Rakel: Conn’s Current Therapy 2001, 53rd ed., W. B. Saunders Co.
10. Ruddy: Kelley’s Textbook of Rheumatology, 6th ed.,2001 W. B. Saunders Company
11. EC Janowsky et al. N Engl J Med Mar-2000; 342(11): 781-790.
12. Wilson: Williams Textbook of Endocrinology, 9th ed.,1998 W. B. Saunders Company
13. KS Pena et al. Am Fam Physician 2001; 63(9): 1763-1770.
14. LM Apantaku Am Fam Physician Aug 2000; 62(3): 596-602.
15. Noble: Textbook of Primary Care Medicine, 3rd ed., 2001 Mosby, Inc.
16. Goroll: Primary Care Medicine, 4th ed.,2000 Lippincott Williams & Wilkins
17. St. Paul’s Hosp. Contin. Educ. Conf. Nov. 2001,Vancouver/BC
18. Gabbe: Obstetrics – Normal and Problem Pregnancies, 3rd ed., 1996 Churchill Livingstone, Inc.
19. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 251.
20. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 250.
21. Ignaz P Semmelweiss: “Die Aetiologie, der Begriff und die Prophylaxis des Kindbettfiebers” (“Etiology, the Understanding and Prophylaxis of Childbed Fever”). Vienna (Austria), 1861.
22. Rosen: Emergency Medicine: Concepts and Clinical Practice, 4th ed., 1998 Mosby-Year Book, Inc.
23. Mandell: Principles and Practice of Infectious Diseases, 5th ed., 2000 Churchill Livingstone, Inc.
24. Horner NK et al. J Am Diet Assoc Nov-2000; 100(11): 1368-1380.
25. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
26. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevier