Introduction
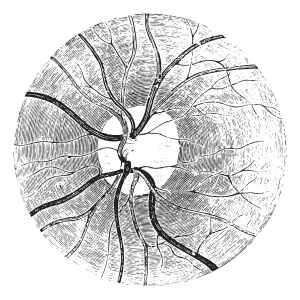
Optic neuritis (also known medically as “papillitis”) is an inflammation of the optic nerve head that is visible with the ophthalmoscope as a yellow disc.
It usually presents on one eye only. The physician finds this most commonly multiple sclerosis, where it is due to demyelination of the optic nerve.
However, temporal arteritis that is associated with polymyalgia rheumatica can also lead to an acute inflammation of the optic disc (optic neuritis). There are many other illnesses that can cause optic neuritis.
Signs and symptoms
There is visual loss on one eye that can present as a blind spot or that involves eventually all of the visual field of the affected eye. Blindness can develop rapidly within 1 or 2 days. The physician notices that the pupillary reflex to light of the affected eye is missing or quite weak. The patient does not feel any pain with this, quite in contrast with retrobulbar neuritis, where pain is prominent.
Diagnostic test
Using the ophthalmoscope the eye specialist sees swelling (=edema) of the optic disc and increased size of the blood vessels (=hyperemia) in an early stage. Later there is more inflammation and there can even be some bleeding form leaking blood vessels. An MRI scan in the case of a multiple sclerosis patient in this image shows a demyelinated optic nerve (left upper arrow) with the other one being normal. It also shows in this case a single demyelinated lesion in the brain, typical for MS (right lower arrow).
Treatment
The physician treats the underlying cause. In the case of multiple sclerosis it has been shown in this study and others that early interferon treatment can make a difference in some patients. Intravenous corticosteroid treatment can shorten the disease process and can reduce the risk of subsequent multiple sclerosis development Ref.6).
References
1.The Merck Manual: optic neuritis
2. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
3. Rakel: Conn’s Current Therapy 2004, 56th ed., Copyright © 2004 Elsevier