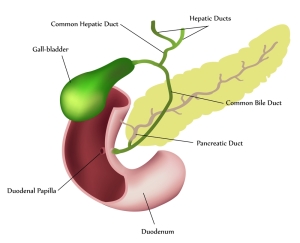
In milder cases treatment of acute pancreatitis consists of hospitalizing the patient and placing the patient on intravenous fluids without any fluids or food by mouth.
By fasting, the gut rests and the gastrointestinal tract ceases to produce secretin and cholecystokinin, two hormones that would have stimulated the pancreas to produce lots of pancreatic juice. A nasogastric tube is being used to suck out any gastric juice as this too will help to settle the pancreatic activities.
Some mortality statistics of acute pancreatitis
Often within a few days the pancreatitis settles down. For most cases the mortality rate is less than 4 to 5%. However, the severe cases described above can have a mortality rate of 15 to 20%. Simchuk et al.( Ref. 6) found that with a CT severity index of 5 or more patients were 17 times more likely to have a longer hospital stay.
They were 10 times more likely to need surgery (resection of dead tissue called “necrosectomy”) and 8 times more likely to die from their severe acute pancreatitis. In these more severe cases treatment needs to be done in the ICU setting and people need to fast for 2 to 4 weeks. This usually requires intravenous nutrition. These patients often have cardiovascular complications due to pancreatic enzymes that have leaked into the system.
Complications of acute pancreatitis
Lung function is suboptimal as lung tissue is very sensitive to phospholipase A2, which originated from the pancreas and traveled via the blood steam to the lungs and damaged them in the process. Blood sugar values have to be watched as in these severe cases the endocrine apparatus in the pancreas( the Langerhans cells) is also damaged. On the other hand blood sugars must not be controlled too closely as these patients are extremely sensitive to developing low blood sugar (hypoglycemia) after insulin injections. This is so because glucagon, another pancreatic hormone which stabilizes blood sugar, is usually no longer produced in the pancreas after severe damage. Many times, because of tissue damage around the pancreas there is leakage of bacteria from the gut such as E. coli and this can quickly lead to a dangerous sepsis and shock.
Intravenous antibiotics and tissue necrosis
Intravenous antibiotics have to be utilized and all of the medical staff have to work very hard to rescue this very sick patient. You can easily see that often so many problems happen at the same time that there one point is easily reached beyond which there is no more help. If there is a sign that the patient might be helped with surgery, a CT scan is usually done, the amount of fluid around the pancreas and the area of tissue necrosis is defined. Ref. 8 showed that the fluid in the vicinity of the pancreas was a better predictor to decide to do surgery than the amount of dead pancreatic tissue.
Minimum procedure to remove dead tissue
This helps the surgeon to plan the appropriate procedure. Often the best procedure is to just do the minimum that has to be done to remove dead tissue and to drain the pancreas into a nearby bowel structure. There are some more fancy Latin words (more doctor language) for some of these procedures, but this would be too technical.
References
1. M Frevel Aliment Pharmacol Ther 2000 Sep (9): 1151-1157.
2. M Candelli et al. Panminerva Med 2000 Mar 42(1): 55-59.
3. LA Thomas et al. Gastroenterology 2000 Sep 119(3): 806-815.
4. R Tritapepe et al. Panminerva Med 1999 Sep 41(3): 243-246.
5. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapters 20,23, 26.
6. EJ Simchuk et al. Am J Surg 2000 May 179(5):352-355.
7. G Uomo et al. Ann Ital Chir 2000 Jan/Feb 71(1): 17-21.
8. PG Lankisch et al. Int J Pancreatol 1999 Dec 26(3): 131-136.
9. HB Cook et al. J Gastroenterol Hepatol 2000 Sep 15(9): 1032-1036.
10. W Dickey et al. Am J Gastroenterol 2000 March 95(3): 712-714.
11. M Hummel et al. Diabetologia 2000 Aug 43(8): 1005-1011.
12. DG Bowen et al. Dig Dis Sci 2000 Sep 45(9):1810-1813.
13. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999.Chapter 31, page 311.
14. O Punyabati et al. Indian J Gastroenterol 2000 Jul/Sep 19(3):122-125.
15. S Blomhoff et al. Dig Dis Sci 2000 Jun 45(6): 1160-1165.
16. M Camilleri et al. J Am Geriatr Soc 2000 Sep 48(9):1142-1150.
17. MJ Smith et al. J R Coll Physicians Lond 2000 Sep/Oct 34(5): 448-451.
More references
18. YA Saito et al. Am J Gastroenterol 2000 Oct 95(10): 2816-2824.
19. M Camilleri Am J Med 1999 Nov 107(5A): 27S-32S.
20. CM Prather et al. Gastroenterology 2000 Mar 118(3): 463-468.
21. MJ Farthing : Baillieres Best Pract Res Clin Gastroenterol 1999 Oct 13(3): 461-471.
22. D Heresbach et al. Eur Cytokine Netw 1999 Mar 10(1): 7-15.
23. BE Sands et al. Gastroenterology 1999 Jul 117(1):58-64.
24. B Greenwood-Van Meerveld et al.Lab invest 2000 Aug 80(8):1269-1280.
25. GR Hill et al. Blood 2000 May 1;95(9): 2754-2759.
26. RB Stein et al. Drug Saf 2000 Nov 23(5):429-448.
27. JM Wagner et al. JAMA 1996 Nov 20;276 (19): 1589-1594.
28. James Chin, M.D. Control of Communicable Diseases Manual. 17th ed., American Public Health Association, 2000.
29. The Merck Manual, 7th edition, by M. H. Beers et al., Whitehouse Station, N.J., 1999. Chapter 157, page1181.
30. Textbook of Primary Care Medicine, 3rd ed., Copyright © 2001 Mosby, Inc., pages 976-983: “Chapter 107 – Acute Abdomen and Common Surgical Abdominal Problems”.
31. Marx: Rosen’s Emergency Medicine: Concepts and Clinical Practice, 5th ed., Copyright © 2002 Mosby, Inc. , p. 185:”Abdominal pain”.
32. Feldman: Sleisenger & Fordtran’s Gastrointestinal and Liver Disease, 7th ed., Copyright © 2002 Elsevier, p. 71: “Chapter 4 – Abdominal Pain, Including the Acute Abdomen”.
33. Ferri: Ferri’s Clinical Advisor: Instant Diagnosis and Treatment, 2004 ed., Copyright © 2004 Mosby, Inc.
34. Suzanne Somers: “Breakthrough” Eight Steps to Wellness– Life-altering Secrets from Today’s Cutting-edge Doctors”, Crown Publishers, 2008